Ketamine is a fast-acting and powerful anesthetic, which induces a trance-like state while providing analgesia (pain relief), sedation, and amnesia (memory loss).
As such, ketamine is not only useful as a sedative, but can also have potential in clinical settings, and even has therapeutic potential—including perhaps as a treatment of negative symptoms associated to autism.
What it does
Ketamine is an NMDA receptor antagonist, meaning it binds to and blocks (i.e. inhibits) the N-Methyl-D-aspartate receptor, called NMDAR. As a result, ketamine induces a state called dissociative anesthesia, which is characterized by the aforementioned analgesia, sedation, amnesia, as well as catalepsy (rigidity of limbs), and a distorted perception of sight and sound, and a feeling of detachment from the environment and self, called dissociation. For a more comprehensive overview of the effects, scroll down to the end of this post.
At (dangerously) high doses, ketamine can even produce a so-called K-hole. More on that later. First, let’s discuss the different uses of ketamine.
Uses of Ketamine
The experience of ketamine for autistic people more or less depends on what the reason for taking ketamine is. Some of the (potential) uses of ketamine are:
- A treatment for symptoms of depression.
- A treatment for PTSD & OCD (potentially).
- A treatment for symptoms related to autism (potentially).
- A preoperative sedative.
- A treatment for substance use disorders.
- For recreational use.
Treatment for depression
Both anecdotally and clinically, Ketamine has shown to have great potential in alleviating symptoms of depression.
Ketamine has also been proven to be a successful antidepressant treatment,[1]Antidepressant effects of ketamine in depressed patients so it is probable that the use of ketamine can help autistic people as well, either as a way of managing autism symptoms, or alleviating symptoms of depression.
Ketamine can also be useful as a pharmacological treatment for treatment-resistant depression (TRD).[2]Ketamine for Treatment-Resistant Depression: A Gateway to Novel Treatment Approaches
Autism treatment
Ketamine has also been purported by some as a possible treatment for autism.
Research from 1991 that looked at the treatment potential of ketamine for autism and other pervasive developmental disorders in children indicates the following:[3]Treating autism and other developmental disorders in children with NMDA receptor antagonists
The effect of the anesthesia lasted about 1 hour after the intravenous drip was discontinued, but the improvement in behavior lasted from five to fifteen days after the administration of the anesthesia.
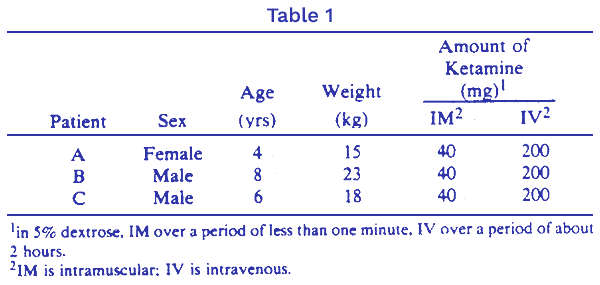
This is what the researcher, Andrew Zimmerman, stated about the three patients that were administered ketamine:[4]Treating autism and other developmental disorders in children with NMDA receptor antagonists
- Patient A was calm over 2 days and then became gradually and increasingly upset with frequent crying as was her baseline.
- The beneficial effects lasted approximately 5 days after the anesthesia.
- Patient B was somewhat lethargic on the first day following the administration of the ketamine but by the second day he was alert, calmer and had a marked decrease in self-abusive behavior.
- Within 10 days of the administration of the ketamine, patient B had learned two new words: “Night-Night” and “bathroom”.
- The improvement lasted for a period of 12 days.
- Patient C became more alert and responsive during the 2 week period following the administration of the ketamine.
No side-effects were seen in any of the patients.
A study from 2015 that looked at ketamine and core symptoms of autism indicates:[5]Ketamine and the core symptoms of autism
Here, we present a single case study in which a patient with a severe intellectual disability was said to have demonstrated a dramatic—albeit short-lived—remission of the core symptoms of autism following adventitious treatment with ketamine.
Although this anecdote is encouraging, we argue that further analysis of ketamine as a treatment for autism is needed.
The effects reported in this 2015 study seem to correspond with the study from 1991. So the beneficial effects don’t last that long, but relatively frequent or even sporadic use of ketamine seems to have the potential to alleviate negative symptoms, and may improve quality of life and mental health.
PTSD & OCD treatment
Although the literature on this is sparse, ketamine and other glutamatergic drugs* have been slowly gaining traction in the psychiatric realm for the treatment of conditions such as post-traumatic stress disorder (PTSD) and obsessive–compulsive disorder (OCD).[6]Beyond Depression: Ketamine and Glutamatergic Agents for PTSD, OCD, and Other Potential Applications
- Glutamatergic drugs either act on ionotropic receptors (especially the NMDA receptors) or modulate glutamate neurotransmission through other mechanisms.
Ketamine—unlike some other glutamatergic drugs—was not found to be particularly useful when it comes to OCD, however, as only a transient decrease in OCD symptoms were observed, unlike depressive symptoms which had a more significant improvement.[7]Augmentation strategies in obsessive–compulsive disorder[8]Effects of ketamine in treatment-refractory obsessive-compulsive disorder
Note also that OCD has considerable overlap with autism. The prevalence of OCD among autistic children ranges from a reported 8% from a study in 2008,[9]Psychiatric disorders in children with autism spectrum disorders: prevalence, comorbidity, and associated factors in a population-derived sample to a prevalence of 37.2% according to a study from 2006.[10]Comorbid Psychiatric Disorders in Children with Autism: Interview Development and Rates of Disorders A systematic literature review and meta-analysis from 2018 by Vuijk et al. reported a prevalence of OCD in autistic adults of 31%.[11]Temperament, Character, and Personality Disorders in Adults with Autism Spectrum Disorder: a Systematic Literature Review and Meta-analysis
As for PTSD among autistics, although I have not been able to find a prevalence rate, research suggests autism shows vulnerability markers for PTSD,[12]PTSD and autism spectrum disorder: Co-morbidity, gaps in research, and potential shared mechanisms and that the occurrence of PTSD may be quite high among autistic people. Read the posts below for more information.
The link between autism & PTSD | The autistic brain & PTSD
So while the efficacy of ketamine may be limited in particular conditions or disorders, due to the co-occurrence of conditions, ketamine may still have beneficial effects in certain areas. With potential in depression, PTSD, and autism combined, ketamine treatment could have a potentially profound impact on those that are affected by all three of the conditions, and I suspect ketamine could also have a use in treating alexithymia, though I have not seen any literature on this.
Anesthetic
Ketamine has also been found to be a good anesthetic when it comes to managing autistic children pre-operation.
Specifically, oral ketamine (6–7 mg/kg) has been found to be the most reliable preoperative sedative for these patients.[13]The anaesthetic management of autistic children
When it comes to children with severe autism, mixing Ketamine with a drink of the child’s choice—Dr Pepper for instance—is one way to administer Ketamine without inducing stress in the child, as a case study from 2009 reports:[14]Combination of oral ketamine and midazolam as a premedication for a severely autistic and combative patient
A 16-year-old, 80-kg, 190-cm-tall male with severe autism was scheduled for dental rehabilitation under general anesthesia. During a dental rehabilitation procedure under general anesthesia 1 year previously, the patient had refused to cooperate and drink his premedication and had become very agitated in the preoperative holding area. This necessitated physical restraint and forcible intramuscular injection with ketamine to sedate him.
On the day of the dental procedure [1 year later], the patient was pacing back and forth in his pre-operative room and appeared anxious. He was clearly agitated and withdrew to a corner when the anesthesiologist entered his room. He even punched one of the nurses when she tried to talk to him.
However, he refused to take the oral premedication mixed in sweet syrup. Learning that Dr Pepper was one of his favored beverages, we mixed the oral medications with 15 ml of Dr Pepper to mask the appearance and change the flavor of the drug. In this disguised form, the patient took the drug readily from his parents. He was then left undisturbed in his bed, and he fell asleep in 20 min.
Individualized perioperative plan
Research from 2017 indicates that individualized perioperative plans* are beneficial for sedation of autistic children.[15]Benefits of an individualized perioperative plan for children with autism spectrum disorder
Although the research indicated the majority of autistic children (62%) were not deemed to require sedation, for those who did, a correlation was found between preoperative sedation and severity level of ASD. In other words, the more severe the autistic symptoms, the more sedation was needed:[16]Benefits of an individualized perioperative plan for children with autism spectrum disorder
- Severity Level 1 (21%) or Asperger’s (31%)
- Severity Level 2 (44%)
- Severity Level 3 (56%)
- Perioperative means everything regarding a patient’s surgical procedure, including ward admission, anesthesia, surgery, and recovery.
Cooperation when administering ketamine roughly correlated with the support levels of autism as well:[17]Benefits of an individualized perioperative plan for children with autism spectrum disorder
- Support level 1 (98%)
- Asperger’s patients (93%)
- Support level 2 (85%)
- Support level 3 (85%)
Substance use treatment
Although ketamine is a drug of potential abuse when used recreationally, its lasting effects without repeated daily use have also shown promise for patients with substance use disorders.
Research from 2018 indicated that ketamine treatment in combination with assisted psychotherapy can help dependent patients in several ways:[18]Considering Ketamine for Treatment of Comorbid Pain, Depression, and Substance Use Disorders
- New perceptions and ideals can be cultivated that are consistent with—and conducive to—sobriety.
- Decreased opiate cravings in patients with substance use disorders may be related to ketamine’s effects on reducing opiate-induced hyperalgesia; hyperalgesia (an increased sensitivity to pain) can counterintuitively emerge in response to opiates.[19]A comprehensive review of opioid-induced hyperalgesia
Given this and additional properties, ketamine can:[20]Considering Ketamine for Treatment of Comorbid Pain, Depression, and Substance Use Disorders
- Help reduce opiate medication burden.
- Augment opiates in the hospice setting.
- Acutely alleviate symptoms of opiate withdrawal.
Recreational use
In addition to its legal use as an anesthetic and potential treatment, ketamine has become a recreational drug in the 1970s, used as a club drug, and, due to its anesthetic properties perhaps more prominently at after-parties.[21]Ketamine | Wayback Machine
Research on the effects of Ketamine for recreational use on autistic people doesn’t seem to exist, but I can offer two anecdotes from autistic people:
Anecdote 1
The music clip that has apparently been playing for 9 minutes just ended.
“What do you think?” I hear someone say from a distance.
I suddenly “wake up” and look around me. I don’t know where I’ve been. I don’t think I was actually present when the music was playing. I dissociated, and my experience became non-local, or abstract.
Now aware, I focus on what I’m feeling, and note that I feel light. I feel like I am a bodiless head on a bedding of clouds. Reality is distant somehow, but intensely present at the same time. I feel warm and fuzzy. Just a head covered in clouds…
“Well?” my friend asks.
“Did you say something?” I respond.
It’s hard to describe what a dissociative experience feels like, but trance-like may be one way of describing it. Below is the music clip mentioned in the first anecdote, which incidentally is also quite representative of the dissociative Ketamine experience.
Anecdote 2
Helen is 19 years old, and has been diagnosed with Asperger syndrome. She is a frequent recreational drug user, and reports that some drugs do not seem to have the same effect on her as in other people.
For example, synthetic psychoactive substances like 2C-B don’t seem to have an effect on her.
She also reports that Ketamine just makes her feel drunk. No dissociation. It does, however, disinhibit her, and causes her to engage in antisocial behaviors such as vandalism.
Effects
In the illustration below, you can see some of the main effects of ketamine.
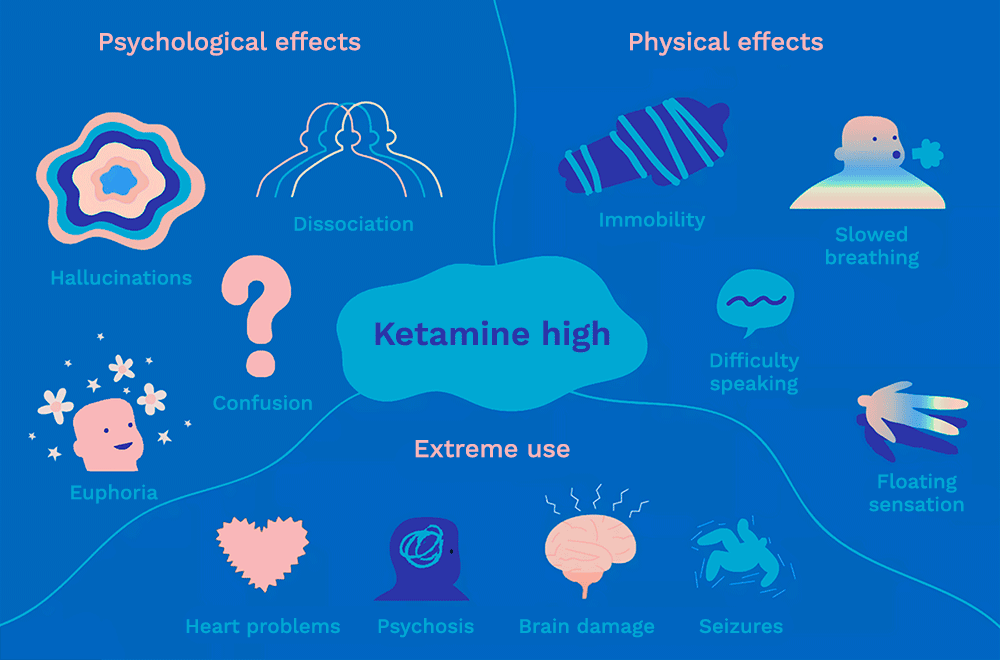
Psychological effects typically produced by ketamine include:[22]What is a K-Hole and How is it Dangerous? | Ketamine
- Hallucinations.
- Out-of-body experiences.
- Disorientation.
- Sense of invincibility.
- Inability to communicate with others.
- Warped thought processes.
- Limited awareness of the surrounding environment.
- Vivid dreams.
Physical effects experienced from ketamine include:[23]What is a K-Hole and How is it Dangerous? | Ketamine
- Inability to perceive pain.
- Slurred speech.
- Loss of coordination.
- Elevated blood pressure.
- Catatonic state.
- Abnormally fast heart rate.
K-hole & risks
Although ketamine has a lot of potential for treatment, and arguably provides pleasant experiences with recreational use, high doses or prolonged use can create unwanted effects.
When injecting ketamine into the muscles, doses of 60–125 mg—or snorting anywhere from 100–250 mg—can produce a so-called K-hole, where your awareness of the world around you as well as your control over your body become so profoundly impaired that you’re temporarily unable to interact with others—or indeed the world around you. As such, you essentially find yourself in a “ketamine-induced hole”—(seemingly) disconnected from the world and others.[24]K Hole and the Awful Effects of Ketamine | Verywell Mind
A K-hole has been reported to be an absolutely dreadful experience; for example, you might think you are dying, and even experience death. Some recreational users deliberately chase the K-hole experience, though this is very dangerous, because overdosage can be fatal.[25]What is a K-Hole and How is it Dangerous? | Ketamine
Side effects often experienced on ketamine include:[26]What is a K-Hole and How is it Dangerous? | Ketamine
- Delirium.
- Chest pains.
- Psychosis.
- Seizures.
- Paranoia.
- Vomiting.
- Severe anxiety.
The state of paralysis that a K-hole can induce can potentially shut down a person’s respiratory and circulatory functions. Ketamine-induced vomiting, in combination with paralysis, can also lead to potential asphyxiation.[27]What is a K-Hole and How is it Dangerous? | Ketamine
Furthermore, the dissociative experience can disconnect one from the self or their environment to such a degree that users may risk injury or fatality.[28]What is a K-Hole and How is it Dangerous? | Ketamine For more information on K-holes, have a look at:
K Hole and the Awful Effects of Ketamine
And lastly, prolonged use of ketamine can lead to ketamine bladder syndrome, the effects of which include incontinence, haematuria (the presence of blood in urine), and profound abdominal pain, and can result in extensive, irreversible damage to the bladder and urinary tract.[29]Participants’ experiences of ketamine bladder syndrome: A qualitative study
As such, before you turn to the street for ketamine, you may want to inquire your local doctor about regulated treatments.
You might also be interested in:
Comments
Let us know what you think!